Blog
Patient Engagement in 2019: Can it Impact Patient Outcomes?
This is the first in a three-part series on patient engagement.
The phrase “patient engagement” started trending around 2011 due to the Patient Protection and Affordable Care Act (PPACA) of 2010. At that time, I co-wrote a paper, The Top Ten Things You Need to Know about Engaging Patients, for the Institute for Health Technology Transformation (now called HIT Summit).
When patient engagement started trending in 2011
- U.S. healthcare costs were $3 trillion and 16.5 percent of people were uninsured.
- The move toward value-based reimbursement was generating a lot of interest in accountable care organizations (ACOs).
- New payment models based on patient outcomes were viewed with a combination of dread and optimism.
In 2011, many of us had high hopes of patient engagement making a difference in a pretty bleak picture of healthcare in the United States.
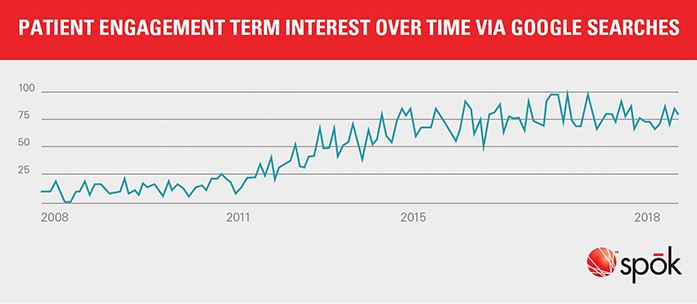
What has changed since 2011?
Fast forward to 2019:
- U.S. healthcare costs have increased to $3.65 trillion.
- After initial progress, reducing the rate of uninsured has started to dissolve. In 2016, the rate had decreased to 10.9 percent. At the end of 2018, the rate was back to 13.7 percent (a four-year high).
- ACOs and ACO contracts continue to rise. At the end of 2018, about 10 percent of the U.S. population is covered by an ACO.
- A total of 48 states are implementing value-based care models, with half of them being multi-payer in scope.
How has patient engagement evolved in the past eight years? First, let’s discuss the term patient engagement.
What is patient engagement, really?
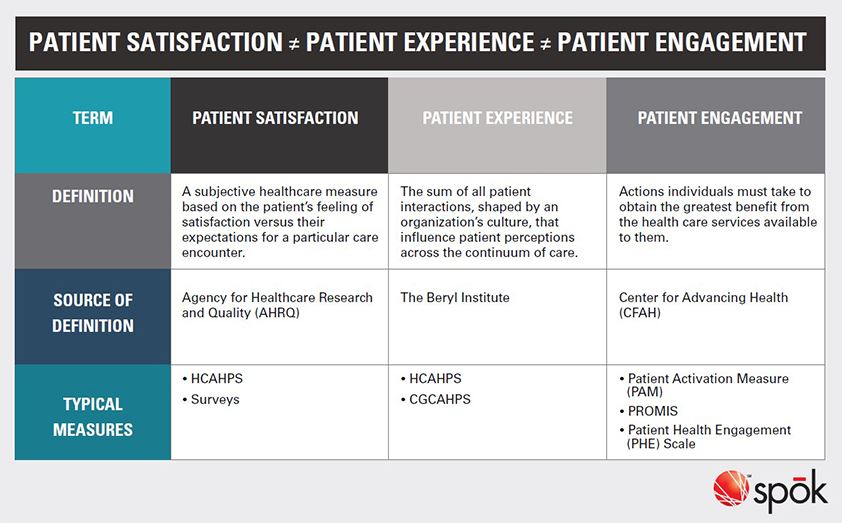
Let’s clarify the difference between three different but related terms: patient engagement, patient satisfaction, and patient experience. The three terms frequently get used incorrectly and interchangeably these days.
See how technology can improve your HCAHPS scores: View the eBrief now.
If you’re looking for a resource on patient engagement versus patient experience, this article also does a nice job of clarifying the difference.
At the risk of oversimplifying, here is my summary of what patient engagement is and what it isn’t.

This table reflects the idea that at the heart of patient engagement, and even patient safety, are communication and collaboration. Patient engagement is not just technology or one, single solution. Rather, it’s the measure of how patients engage with all the resources their health system makes available to them.
Can Patient Engagement Have a Positive Impact on Patient Outcomes?
The research since 2011 on the impact of patient engagement suggests it can indeed positively impact outcomes.
One of the most useful studies is the 2013 Hibbard patient activation measure (PAM) study. In 2013, the PAM measurement approach was relatively unknown to hospital staff and certainly to physicians at that time. But this early study using PAM as the key metric showed that patient engagement can indeed “move the needle,” and in some cases, significantly.
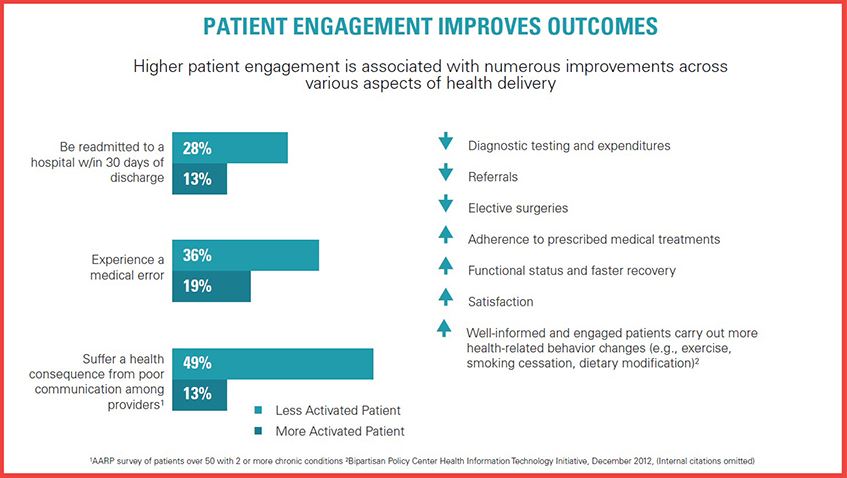
Additionally, there is other research since 2011 that confirms the PAM study findings. Some of these studies include:
Healthcare action plans assist in patient outcomes
- In July 2013, published research in Chronic Illness examined how healthcare action planning and details of health action plans helped achieve improved patient outcomes. The conclusion reads, “Action planning appears to be an important component of self-management interventions, with successful completion associated with improved health and self-efficacy outcomes.”
- In 2018, the Patient-Centered Outcomes Research Institute (PCORI) and Boston Children’s Hospital researched if an increase in parent engagement associated with their children would reduce hospital medical errors for pediatric patients. The hospital implemented a new verbal communication plan, called I-PASS, which included a discussion of what the family and staff should expect. The plan was deployed during daily hospital rounds. This reduced “harmful medical errors” by 38 percent in the study of more than 3,000 patients. It is the “first multicenter study to show that a family-centered communication program directly improves hospital safety.”
Correlation between self-efficacy engagement and healthcare results
- Stanford University published research in 2014 showing a significant correlation between patient engagement in the form of “self-efficacy” and the patients’ healthcare results. In this case, self-efficacy referred to a patient’s “perceived capability to perform specific actions required to achieve concrete goals.”
Using technology to increase patient engagement
- In 2016, a study published in the Journal of Medical Internet Research shows that mHealth apps can help remind diabetic patients to build healthy habits, which improves chronic disease management.
- In 2016, Stanford and the University of Hawaii Cancer Center studied the link between patient outcomes and program engagement, action planning completion, and program personalization. The study found among its 350 participants: “Active involvement and interaction in the form of posting is associated with larger improvement in outcomes. Specifically, we found that those who posted the most also appeared to get the most benefit.”
- In 2017, a study by Tractica showed correlation between patient engagement and proactive wellness behaviors. The study concluded that: “When patients are fully engaged in their care, they are more likely to maintain treatment plans, track their health, and ask their providers questions. These behaviors will ideally prevent an illness from getting worse and resulting in more costly and invasive interventions.”
These studies and others indicate that patient engagement under certain conditions can, in fact, move the needle on improving healthcare. In the next part of this blog series, I will explore two initiatives that can drive effective patient engagement. If you’re interested in staying up-to-date on our newest blog posts, subscribe using the red subscribe button above.








