All resources
Search resources
Filter by topic
Filter by role
Filter by solution
Filter by type
{content}
Resource
Webinars
Fragmented systems hinder healthcare. Join Spok to see how a unified platform integrates enterprise data and enhances clinical communication for seamless workflows and better patient outcomes.
Resource
Infographics
Tired of the constant "beeps and alerts" in healthcare? Alert fatigue and alarm management are critical challenges, but your care team can overcome them. Learn the 3 key steps to cut through the noise, reduce clinician burnout, and significantly improve patient safety.
Resource
eBooks and white papers
Feeling overwhelmed by constant beeps and alerts in healthcare? You're not alone. Alert fatigue and alarm management are major challenges, leading to clinician burnout and serious patient safety risks. Dive in to understand the true impact of alarm fatigue and how it's affecting healthcare teams.
Resource
Case studies
VHC Health achieved seamless interoperability with Spok Care Connect, streamlining clinical communication workflows and enhancing patient safety.
Resource
Webinars
Learn from a Spok expert about how optimizing critical test result notifications can improve patient safety and streamline clinical workflows. Register now!
Resource
Videos
See how Spok's comprehensive hospital communication platform streamlines clinical workflows. Connect care teams and technology seamlessly for enhanced patient care coordination.
Resource
Infographics
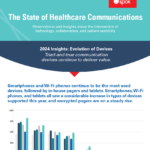
Explore the newest findings from Spok's annual healthcare communication survey, highlighting the use of devices in healthcare organizations in 2024. Delve into significant challenges and strategies for providing outstanding patient care.
Resource
Infographics
Discover the latest insights from Spok's annual survey on healthcare communication, revealing how burnout impacts healthcare organizations in 2024. Explore key challenges and solutions for delivering exceptional patient care.
Resource
Infographics
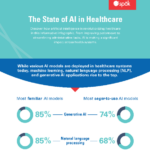
What are the trends, challenges, and predictions for the future of healthcare communications? Get insight into the challenges facing our nation’s health systems and the importance of communication technology for providing excellent patient care.
Resource
Infographics
When critical test results require immediate attention, our solution ensures that the right clinicians receive notifications promptly, acknowledge receipt, and take appropriate action—all within a trackable workflow that documents each step from result generation to clinical intervention.